Low Testosterone: 12 Signs You Have It and 8 Science-Backed Natural Solutions (2026)
Low testosterone affects an estimated 40% of men over 45 — yet most don't recognize the symptoms. Fatigue, low libido, belly fat, and mood changes are often blamed on 'aging' when the real culprit is hormonal. Here's the complete guide.
The Silent Epidemic: Why So Many Men Are Running Low
Here is a statistic that surprises most men: average testosterone levels in men have been declining for decades. A landmark study comparing testosterone levels of men in the 1980s versus equivalently-aged men in the 2000s found testosterone had declined an average of 17% in just two decades — independent of age. A 2020 analysis confirmed the trend continues.
The causes are environmental, psychological, and behavioral: endocrine-disrupting chemicals in plastics (BPA, phthalates), chronic stress elevating cortisol (testosterone's primary antagonist), widespread Vitamin D deficiency, declining sleep quality, sedentary lifestyles, and diets poor in zinc and healthy fats. The result: millions of men experiencing functional testosterone deficiency attributable more to modern environment than to pure biology.
Yet most of these men are told they're "just getting older" and sent home. This guide explains what's actually happening, how to recognize it, and what science-backed strategies are available.
The Biology of Testosterone: Why It Controls So Much
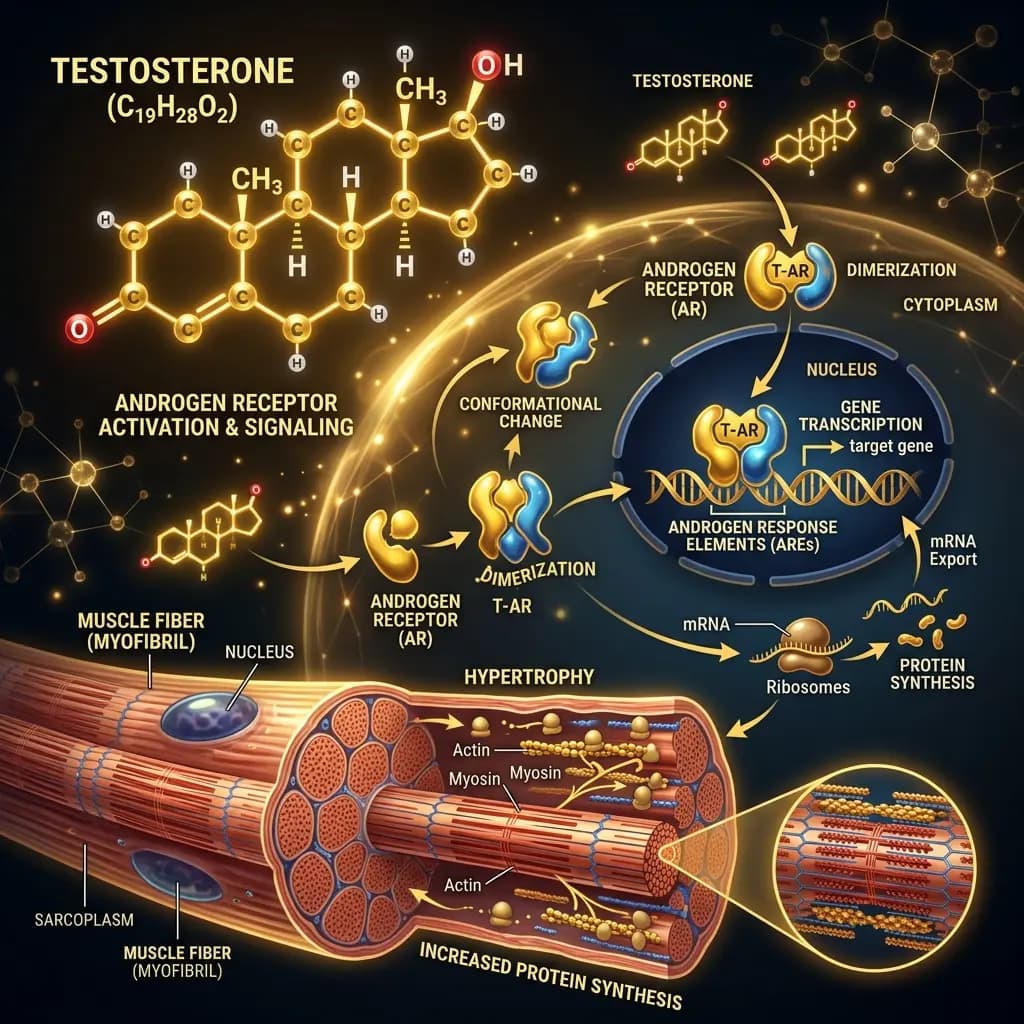
Testosterone is far more than a "sex hormone." It is a master regulatory steroid that influences:
- Muscle: Activates muscle cell gene transcription for protein synthesis, satellite cell activation (muscle repair), and nitrogen retention
- Fat distribution: Promotes lipolysis especially in visceral (abdominal) adipose tissue — low testosterone directly creates the "beer belly" pattern
- Bone density: Stimulates osteoblast (bone-forming) cell activity — low testosterone increases fracture risk and osteoporosis
- Red blood cells: Promotes erythropoietin production and red blood cell formation — contributes to energy and physical stamina
- Brain: Testosterone receptors are distributed throughout limbic (emotional) and prefrontal (cognitive) brain regions — directly influences mood, motivation, focus, and aggression
- Cardiovascular: Supports nitric oxide production and arterial elasticity — healthy testosterone is cardioprotective
- Sexual function: Drives libido, erectile function, and sperm production directly
This is why the symptoms of low testosterone are so diverse and non-specific — testosterone's fingers are in almost every physiological pie.
12 Signs You May Have Low Testosterone
None of these alone confirms low testosterone — but if you recognize multiple, testing is warranted:
- Persistent fatigue that doesn't resolve with rest — not normal tiredness, but a deep, motivational exhaustion
- Reduced libido — noticeably lower sexual desire versus your personal historical baseline (not comparison to others)
- Difficulty building or maintaining muscle despite consistent training — workouts feel less productive
- Increased body fat, particularly abdominal/visceral — waistline expanding despite relatively stable diet
- Mood changes: irritability, low mood, reduced motivation — sometimes described as "emotional flatness" or "I just don't care about things I used to care about"
- Cognitive fog — trouble concentrating, slower thinking, memory gaps
- Reduced exercise performance and slower recovery — workouts that used to feel manageable now feel disproportionately hard
- Erectile dysfunction or reduced morning erections — not absolute dysfunction, but reduced frequency and quality
- Sleep disturbances — difficulty falling asleep or staying asleep, with testosterone ironically needed for deep sleep which also produces testosterone (a negative feedback loop)
- Reduced body hair — particularly on legs, chest, and face
- Testicular changes — reduced size or firmness (often unnoticed)
- Hot flashes or sweating episodes — yes, men experience hormonal night sweats too, particularly during testosterone decline
The Testing Reality: What Numbers Actually Mean
If you recognize 4+ symptoms, request a morning fasting blood test for:
- Total testosterone: Standard reference range is 300-1,000 ng/dL. However "normal range" was calculated across all age groups — a 70-year-old man's "normal" is not appropriate for a 40-year-old
- Free testosterone: Often more clinically relevant than total — sex hormone binding globulin (SHBG) binds testosterone, making it unavailable to receptors. Free testosterone is what actually reaches your cells
- LH (Luteinizing Hormone): High LH with low testosterone suggests primary hypogonadism (testicular issue); low LH with low testosterone suggests secondary hypogonadism (pituitary/hypothalamic issue)
- SHBG: As men age, SHBG increases, binding more testosterone and reducing free testosterone even when total appears adequate
8 Science-Backed Natural Strategies to Optimize Testosterone
1. Optimize Sleep Architecture
The majority of daily testosterone is produced during REM and slow-wave sleep. A landmark study in JAMA found that sleeping 5 hours per night for one week reduced testosterone by 10-15% in young healthy men. Conversely, optimizing sleep duration (7-9 hours) and quality is one of the fastest testosterone optimization strategies available.
Sleep optimization targets: consistent sleep/wake schedule, cool bedroom (65-68°F), no alcohol (disrupts sleep architecture), no screens 90 min before bed, blackout curtains.
2. Resistance Training
Heavy compound lifts (squats, deadlifts, bench press, rows) acutely elevate testosterone during and after exercise. A 2012 meta-analysis in Sports Medicine confirmed resistance training — particularly at high intensity with short rest intervals — produces the most robust hormonal responses. Aim for 3-4 sessions per week with compound movements at 70-85% 1RM intensity. Chronic cardio at excessive volumes can suppress testosterone — balance is critical.
3. Fix Nutritional Deficiencies
Three micronutrient deficiencies directly suppress testosterone:
- Zinc: Required for testosterone biosynthesis. 45% of older men are zinc deficient. Best food sources: oysters (highest), beef, pumpkin seeds, cashews
- Vitamin D: 41% of Americans are deficient. Supplement with 2,000-5,000 IU D3 daily (test serum levels first). Foods: fatty fish, egg yolks, fortified dairy
- Magnesium: Reduces SHBG binding of testosterone, potentially increasing free testosterone. Foods: dark leafy greens, dark chocolate, nuts, seeds
4. Reduce Chronic Stress (Cortisol Antagonism)
Cortisol and testosterone have an inverse relationship in the hormonal hierarchy. Chronic psychological stress maintains elevated cortisol, which directly suppresses gonadotropin-releasing hormone (GnRH) at the hypothalamus — the master signal for the testosterone production cascade. Evidence-based stress reduction: zone 2 aerobic exercise (walking, swimming — not intense cardio which can elevate cortisol), mindfulness, journaling, social connection.
5. Optimize Body Composition
Adipose tissue contains aromatase — the enzyme that converts testosterone to estrogen. Excess visceral fat creates a vicious cycle: low testosterone increases fat, which increases aromatase, which converts remaining testosterone to estrogen, further suppressing testosterone. Even modest fat loss of 5-10% body weight reliably improves testosterone in overweight men.
6. Minimize Endocrine Disruptors
BPA (in plastics) and phthalates (in food packaging and personal care products) are xenoestrogens — compounds that mimic estrogen and compete with testosterone at receptor sites. Practical reduction: glass or stainless water bottles, fresh/frozen food over canned, natural personal care products, avoid heating food in plastic containers.
7. Optimize Fat Intake
Testosterone is synthesized from cholesterol. Low-fat diets have been consistently associated with lower testosterone. Include adequate healthy fats: olive oil, avocado, fatty fish, eggs, nuts. Avoid trans fats and excessive seed oils. A 2021 review confirmed dietary fat composition directly affects testosterone production capacity.
8. Targeted Botanical Supplementation
Several botanical compounds have level-1 evidence for supporting testosterone in men with age-related or lifestyle-related decline:
- Ashwagandha (KSM-66): 14.7% testosterone increase in published RCT; 27-30% cortisol reduction
- Fenugreek Extract: Preserves free testosterone by inhibiting aromatase and 5-alpha reductase — maintaining testosterone availability
- Tribulus Terrestris: LH stimulation supporting endogenous testosterone production; particularly effective for men with sexual function concerns
Products combining these evidence-backed botanicals with zinc and vitamin D — like SpartaMax — offer the most comprehensive supplement approach to multi-pathway testosterone optimization in a convenient daily format.
When to See a Doctor
Natural strategies are appropriate for men with functional, age-related testosterone decline. Seek medical evaluation if:
- Total testosterone is consistently below 300 ng/dL on morning fasting tests
- Symptoms are severe (significant erectile dysfunction, extreme fatigue, pronounced mood disorder)
- You have a history of pituitary/hypothalamic conditions
- You are under 35 with symptoms (early-onset hypogonadism requires investigation)
Medical options including TRT are appropriate in these cases — and a competent endocrinologist will consider natural approaches as complements regardless.
Conclusion: Your Testosterone Is Partly Within Your Control
The evidence is clear: testosterone decline is not purely inevitable biology. Environmental factors, nutritional deficiencies, sleep debt, chronic stress, and sedentary lifestyle all accelerate decline far beyond what age alone predicts. The flipside: addressing these factors through targeted lifestyle changes and evidence-based supplementation can meaningfully restore and maintain testosterone levels that support strength, stamina, and quality of life for decades longer than most men currently achieve.
Start with testing, identify your specific deficiencies and lifestyle factors, then address them systematically — with targeted botanical support from a quality product like SpartaMax as a complement to your foundational lifestyle changes.